 
She had to leave work early on July 3 because of generalized pain and a temperature of 39☌. 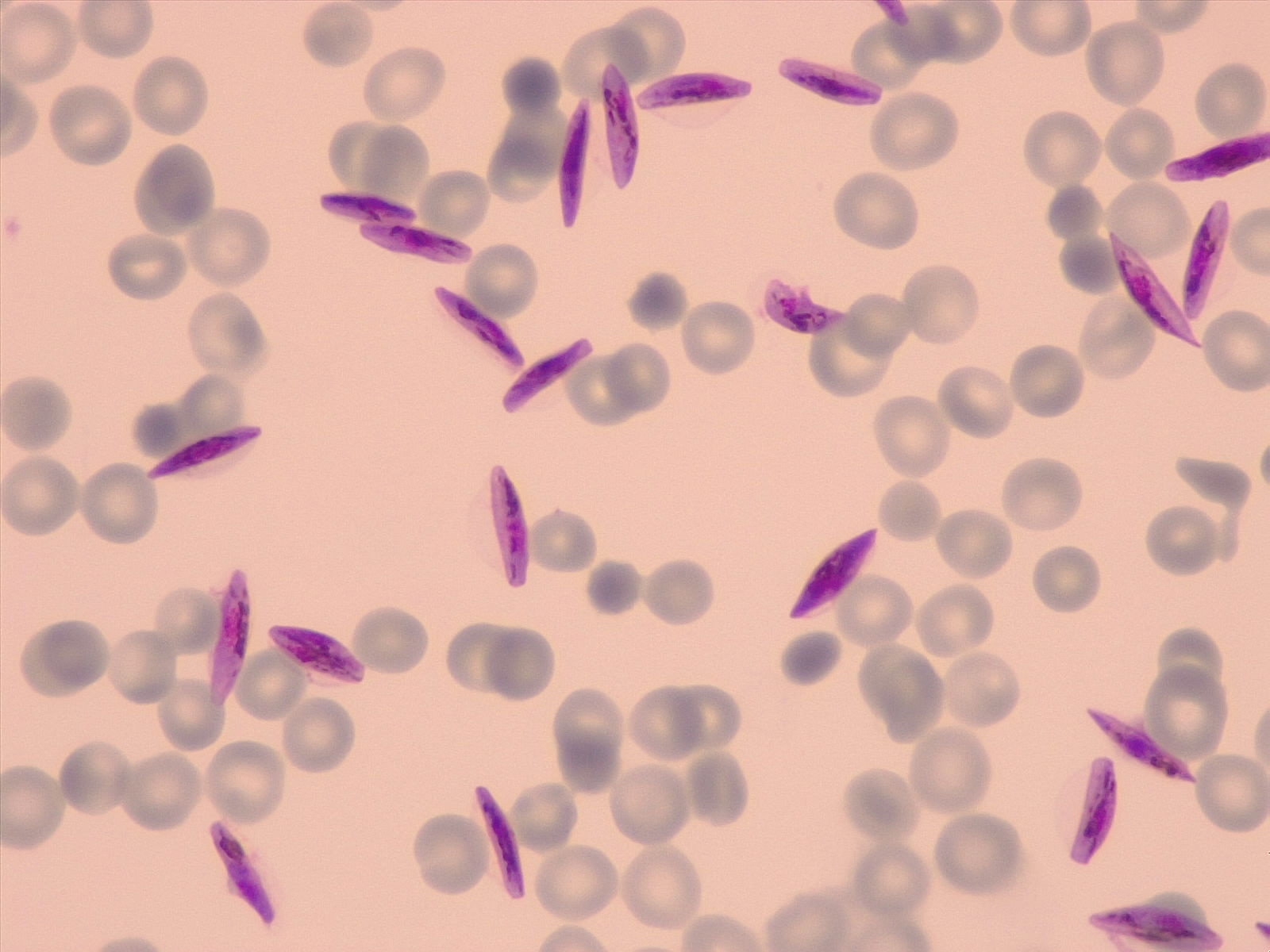
Her condition returned to normal on July 2 before a second bout of fever and myalgia occurred during the night. The injured nurse did not inform the managing physician that the injury had occurred while she was drawing blood from a patient to determine if the patient was infected with malaria.īy July 1, 10 days after exposure, fatigue, malaise, and fever developed her temperature was lowered to 38.6☌ by taking paracetamol. The risk of infection by pathogens other than HBV, HCV, or HIV following a needlestick injury was not discussed during her postexposure interview, and the nurse was not made aware of that risk. In accordance with national postexposure management guidelines, she was tested for HIV and hepatitis C virus (HCV) antibody, and results were negative at baseline her immunization against hepatitis B virus (HBV) was confirmed. She notified the hospital occupational medicine department of her injury on the day it occurred and was given a postexposure interview. She had no previous history of needlestick injury. The needlestick pierced the nurse's glove and caused a deep, blood-letting injury on the anterior aspect of the left wrist. She removed the catheter stylet and stuck herself as she crossed her hands to discard the stylet in a sharps container. On June 21, 2001, she sustained an accidental needlestick injury while taking a blood sample with an 18-gauge, peripheral venous catheter that had no safety feature. She had been certified as a registered nurse on May 28 and had been working as a substitute employee at various hospitals in the greater Paris area. She had vacationed in the south of France from June 23 to June 26 but had traveled by car. She did not live near an airport, nor had she been to one recently. The patient had not traveled outside France except to the United Kingdom years earlier. She recovered completely and was discharged on day 6 of hospitalization. Her malaise persisted for 3 days, but she did not show any signs of malaria. The patient was given 500 mg of oral quinine three times daily intravenous quinine was administered 15 hours after admission because she became nauseated. Result of a blood film to identify Plasmodium falciparum was positive for parasitemia at 0.038 per 100 erythrocytes. Results of an abdominal echogram were normal. Biologic tests indicated normal values except the following: platelets 47.4 x 10 3/µL, aspartate aminotransferase 307 U/L (normal value <56), alanine aminotransferase 239 U/L (normal value <56), total bilirubin 58 µmol/L (normal value <24), and γ-glutamyl transpeptidase 57 U/L (normal value <35). Urinalysis did not show hematuria or signs of urinary infection. She was slightly jaundiced and reported a mild headache but showed no resistance to head flexion. On admission, after she was given paracetamol, her axillary temperature was 37.6☌. She had no notable medical history, except spontaneously regressive Schönlein-Henloch purpura at 9 months of age. To the Editor: A 24-year-old female nurse was admitted to the emergency room at Bichat University Hospital in Paris, France, on July 4, 2001, with fever, nausea, and general malaise. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
